7-year-old girl with rare congenital disease undergoes whole liver transplant in Pune
Jan 19, 2023
Category: News
At Jupiter Hospital, we are equipped with over 30 specialty treatments. There are specialised departments dedicated to illnesses which are backed by skilled and experienced doctors and team of healthcare professionals who are also experts at their craft.
Have a query or need to visit an expert? Book an appointment online to consult our doctors and we’ll take care of your needs.
Established in 2007, Jupiter Hospital is a tertiary care Hospital with a ‘Patient first’ ideology deeply instilled in its foundation, to deliver leading-edge healthcare to cater to the changing needs of the growing populace.
Through Jupiter Foundation, we ensure world class health care for the people that are economically challenged. Jupiter Foundation works on the philosophy of putting the patient first in everything.

At Jupiter, we believe there is a better path to healing that humanizes the practice of health care and inspires hope in the Patient & family who need it most. Our primary value – The needs of the patient come first – is at centre of our plans and decisions. You'll also find that our pride – in where we work, and in what we do – is a common trait. You will be truly part of an amazing team committed to solving the most serious and complex medical challenges.
Eastern Express Highway, Service Rd, Next To Viviana Mall, Thane,
Maharashtra - 400601
Jupiter Hospital, Baner,
Pune.
Scheme No. 94, Sector 1,Ring Road, Near Teen Imli Square,
Indore,
Madhya Pradesh - 452020
Jupiter Hospital, Kalyan Shill Road,
Dombivli 421204

Jan 19, 2023
Category: News
The girl was diagnosed with a liver disease called biliary atresia in which there are no bile ducts in the liver from birth. She received the organ from a 10-year-old boy who died following an accident.
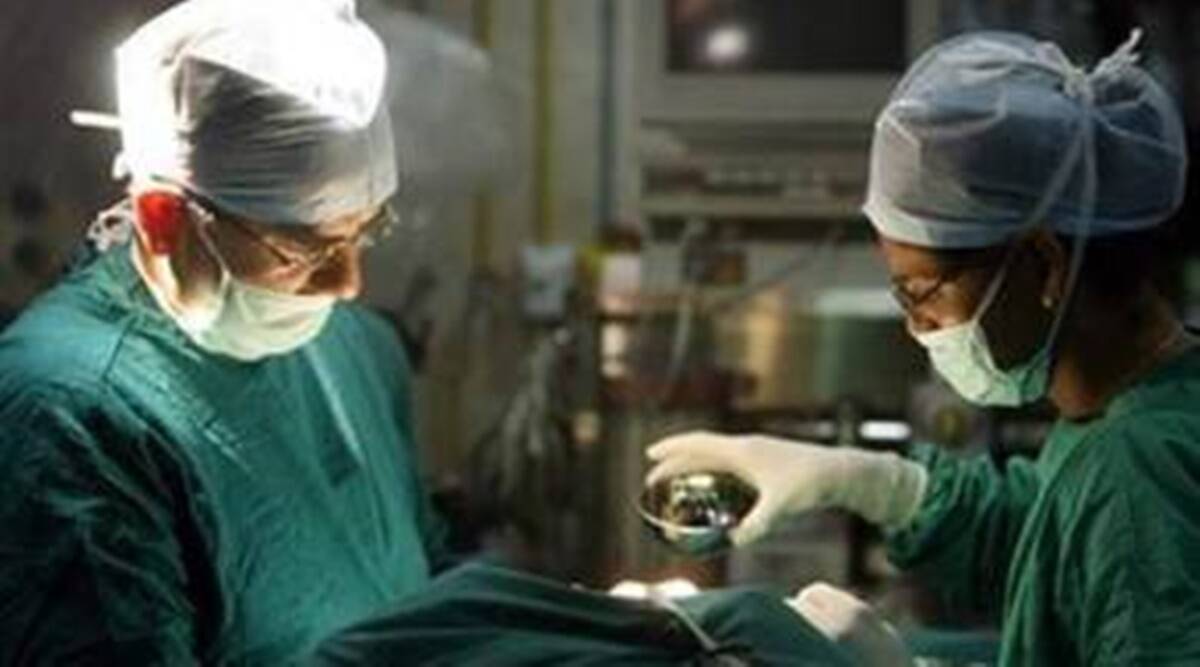
A complicated paediatric whole liver transplant, lasting eight hours, was successfully performed on a seven-year-old girl after she received the organ from a 10-year-old boy who died following an accident, a statement from Jupiter Hospital in Pune said. The patient has recovered well and was discharged within two weeks of the liver transplant, Dr Rajendra Patankar, CEO of the hospital, added.
The girl had increasing jaundice starting from six weeks of age, doctors said. A thorough diagnosis and systematic assessment indicated she suffered from a rare congenital liver disease called biliary atresia where there are no bile ducts in the liver from birth.
In babies with biliary atresia, the flow of bile from the liver to intestine is blocked which can lead to liver damage and cirrhosis, which can be fatal if not treated. Her health was continuously deteriorating. The infant underwent Kasai portoenterostomy (KPE) to connect the liver to the small intestine, going around the abnormal ducts. The procedure is the primary treatment with subsequent liver transplantation in failed cases. Post-surgery many children develop liver cirrhosis in the first or second decade of their life.
“(She) came to us around the age of 5 with complaints of jaundice, weakness and most importantly growth failure. After reviewing the patient’s condition, she was found to have low platelet and albumin levels, oesophageal varices, massive splenomegaly and ascites which presented a classic picture of liver cirrhosis. The child had started decompensating and in the absence of a cure for the ailment, we offered them the option of liver transplant,” said Dr Vishnu Biradar, paediatric gastroenterologist and hepatologist at the hospital.
Unfortunately, her parents and family members were not fit to donate a liver. Though the chances of a suitable liver donor were slim, the patient was listed for a cadaveric donor. After a year, the wait ended. “Once we received a liver donor, our team swiftly handled all the necessary preparations for the surgery,” Dr Biradar said.
Dr Manoj Shrivastava, consultant transplant surgeon at the hospital, said, “Surgery was technically challenging due to previous surgery, small size of blood vessels and bile ducts, and a possibility of size mismatch. Besides, the difference in weight and age presented difficulty in placing the liver in the abdominal cavity. However, the large size of the previous liver and fluid in the stomach helped to close the abdomen without any complications.”
“Recently, we completed more than 25 paediatric liver transplants in patients less than 16 years of age and more than 110 adult liver transplants at Jupiter Hospital,” Dr Patankar added.
News
May 09, 2024
News
Jan 19, 2023